This article breaks down how patient communication actually works in healthcare clinics and hospitals, and why SMS-first models are continuing to be the standard across healthcare providers. While many practices have historically relied on physical mail for patient correspondence, the rising cost of postage and growing focus on sustainability are accelerating the shift toward digital channels. We explore the trade-offs between SMS and email, including how SMS and secure messaging approaches compare, and what a practical, secure communication strategy looks like in real-world healthcare environments.
3 Keys to Implementing Secure Messaging
Email or SMS for healthcare?

Deliverability and Engagement
The most practical difference between SMS and email is how likely the message is to be seen and acted on, and how consistently healthcare providers can achieve successful delivery across systems.
SMS is immediate. Messages are typically opened within minutes and are difficult to ignore. This makes it well-suited to time-sensitive communication, such as sending appointment reminders, an upcoming appointment notification, or prompts requiring action through text messaging.
Email is less predictable. Messages may be filtered into spam, overlooked in crowded inboxes, or opened too late to be useful. In some households and care settings, email accounts are also shared between family members or carers, meaning messages may be missed by the intended recipient. Even when delivered successfully, engagement varies significantly, increasing the risk of missed appointments and gaps in communication.
In practice, health providers tend to rely on SMS when visibility and timing matter, using SMS solutions to communicate critical patient information efficiently, while email is used in more supportive roles across broader clinical workflows.
Data Quality and Capture
The reliability of a communication channel is closely tied to the quality of the data behind it, particularly when managing patient data across healthcare providers and systems.
Mobile numbers are consistently captured and verified during patient registration and admissions. They are always requested for direct contact and are regularly updated through patient interactions, supporting more secure and efficient communication.
Email addresses are less consistent. They may be missing, outdated or infrequently checked. In some cases, patients use shared email accounts, which can introduce additional privacy risks when communicating clinical information. Compounding this, some legacy PAS or eMRs don’t support email capture, and where it has been introduced, there can be a significant lag in populating that data.
This difference matters. SMS benefits from stronger, more reliable data capture, while email introduces variability that can affect delivery, engagement, and contribute to higher clerical error rates across healthcare organisations.
Security & Privacy Expectations
Healthcare communication and secure messaging involves choosing a balance between accessibility with strict privacy requirements, particularly when healthcare providers are handling sensitive clinical information.
Email has traditionally been viewed as less secure due to the risk of shared inboxes and unauthorised access. Once information is sent, control over who views it is limited, reducing security over transmitted patient data.
SMS can be used more safely when structured correctly. In most clinic environments, SMS messages won’t include personally identifiable information (PII) or health information (HII). Instead, they act as notifications, backing secure messaging practices.
Patients can then be prompted to log into a secure portal, where sensitive information is accessed through authentication methods such as one-time passwords (OTP). This first step ensures information is accessed securely within a controlled environment, often reinforced by encrypted systems found in most clinical software.
This separates the notification layer from the secure information layer, reducing exposure while maintaining usability and enabling a more secure exchange of important information across systems.
The Five Faces Model: Why SMS-First Works

In practice, the most effective approach we see is an SMS-first communication model supported by a secure digital front door.
Secure messaging via SMS is used for simple, high-impact interactions. This includes appointment reminders, notifications, and prompts to log into a patient portal. Messages can remain generic and avoid containing sensitive information.
All detailed communication should be accessed through a patient portal or hub. This includes appointment details, forms, educational material and patient-specific information. Access is controlled through secure authentication. Once in the patient portal/hub, patients can also initiate messages via a secure, in-platform inbox, ensuring confidentiality and traceability.
This model aligns with familiar digital experiences, such as government services where users receive a notification and log in to access details. Patients understand this pattern, which reduces friction and improves engagement.
For healthcare providers, it creates a clear separation between communication and information delivery, allowing both to be managed more effectively across multiple systems.
Where Email Still Fits in Healthcare Communication
Email still plays a role, but it is typically not the primary channel.
It is best suited to non-urgent communication where immediacy is not required. This includes general updates, educational content, and pre- or post-care information that does not contain sensitive data within a broader patient engagement communications strategy.
Email can also act as a secondary channel, supporting SMS or serving as a fallback when SMS delivery is unsuccessful. However, its limitations are important to acknowledge. Engagement is lower, deliverability is less predictable, and it is not well-suited to time-sensitive workflows.
In most hospital environments, email works best as a complementary channel rather than a primary one.
The Hidden Challenge: “Letting Patients Choose” Their Channel
Allowing patients to choose their preferred communication channel appears patient-centric, but can actually introduce operational complexity. Patients often assume that their preference applies across the entire health service. In reality, most hospitals operate multiple disconnected systems, each managing communication differently. Preferences are rarely synchronised across these systems.
This leads to inconsistent experiences, where patients may receive SMS from one system and email from another.

It also increases the risk of missed communication, particularly when preferences are not applied consistently. In practice, a standardised communication approach is often more effective than attempting to manage fragmented preferences. Consistency improves both operational efficiency and patient outcomes and is supported by integrated patient engagement solutions.
When to Use SMS vs Email: A Decision Framework
For most healthcare providers and clinical practices in the healthcare industry, the decision comes down to urgency, action and reliability.
| Scenario | Use SMS | Use Email |
|---|---|---|
| Time Sensitivity | High urgency (same day, next day, time-critical) | Low to moderate urgency |
| Action Required | Yes – confirm, attend, log in, respond | No immediate action required |
| Visibility Needed | High – message must be seen quickly | Moderate – can be read later |
| Type of Content | Short, prompt-based communication | Longer-form or informational content |
| Patient Engagement | When engagement is critical | When reinforcing or supplementing SMS |
| Examples | Appointment reminders, check-in prompts, portal login links | Pre/post care info (non-sensitive), general updates, education |
Failover Strategy: Why You Shouldn’t Rely on One Channel
No communication channel is completely reliable.
SMS failures are uncommon but possible. Email failures are more frequent due to spam filtering, incorrect addresses, or low engagement.
Relying on a single channel increases the risk of missed communication. In healthcare, this risk affects both operations and patient care.
A failover strategy reduces this risk and can be further strengthened by digital health patient experience solutions. SMS is typically used as the primary channel, with email or the patient portal/hub itself acting as a secondary fallback. If one channel fails, the other can reinforce the message.
This approach improves contact rates and supports more consistent patient engagement.
Audit Trails and Compliance in Patient Communications
Healthcare communication must be traceable.
Practices need visibility over what was sent, when it was sent and how patients interacted with it. This includes delivery status, timestamps or other actions such as logins or confirmations.
Audit trails support clinical governance, provide legal protection and enable operational reporting. They also allow teams to identify communication gaps and improve performance over time. Without this visibility, it is difficult to ensure accountability or demonstrate compliance.
Australian Privacy Considerations
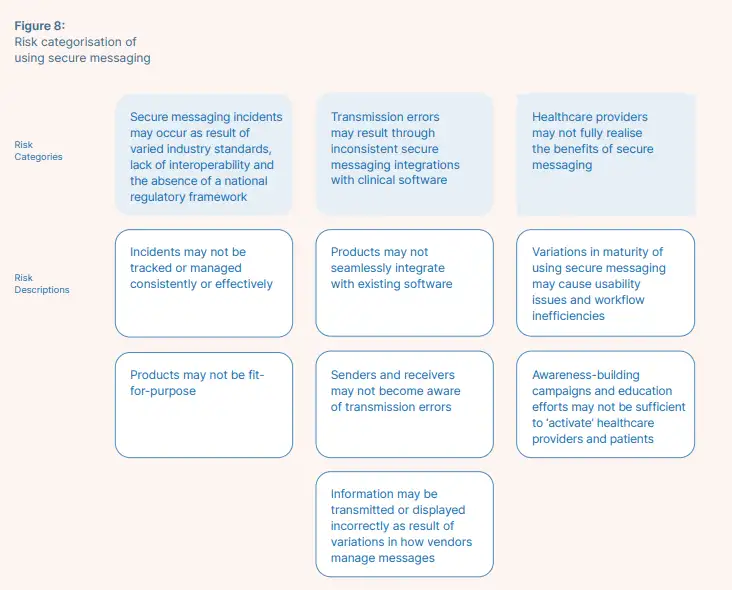
Graphic Source: Australian Digital Health Agency, Safety and Quality Benefits of Secure Messaging
Healthcare organisations in Australia must align communication practices with the Australian Privacy Principles (APPs).
A key requirement is limiting the exposure of sensitive information. SMS and email should not include personally identifiable or health information wherever possible.
Instead, sensitive data should be accessed through secure portals with appropriate authentication, such as OTP-based login.
Consent must also be captured and recorded. Patients must agree to receive communications, and documented preferences must be managed appropriately.
An SMS-first, portal-based model, supported by a secure patient hub, meets these requirements by reducing exposure while maintaining accessibility.
SMS for Healthcare Communication Compliance Checklist
| ☐ | No sensitive patient data in SMS or email messages |
| ☐ | Patient consent captured and recorded |
| ☐ | Messages directing patients to a secure portal |
| ☐ | Audit logs enabled across all communications |
| ☐ | A clear, standardised channel strategy |
| ☐ | A failover process for delivery issues |
| ☐ | Data handling aligned with Australian regulations |
Building a Scalable Patient Communication Strategy
As healthcare continues to digitise patient engagement, communication needs to be coordinated across systems rather than managed in isolation.
A common challenge is the lack of a centralised communication layer. Messages are sent from multiple platforms, each operating independently, which creates inconsistency and inefficiency.
A more scalable approach is to connect these systems through a unified digital front door. This allows communication to be triggered across systems while maintaining a consistent patient experience. Prompting patients via SMS to provide feedback via the secure patient hub or a feedback tool can further support continuous improvement and patient satisfaction, helping teams refine their approach over time. Find out more about our solutions today by getting in touch with the Five Faces team.
Supporting Sources:
Australian Digital Health Agency (2020), Safety and Quality Benefits of Secure Messaging